Medicare is a mainstay of retiree health care, but its “Parts” can be difficult to divine. So if you’re frustrated because you don’t understand how Medicare Part C (aka Medicare Advantage) works, don’t worry—you’re hardly alone.
When Medicare came about in the 1960s, it originally consisted of Parts A and B (hence its nickname, Original Medicare). Part C didn’t come around until the 1990s; it was initially called Medicare+Choice, but it has since changed to Medicare Advantage. Indeed, nowadays, we use the terms Part C and Medicare Advantage interchangeably.
Part C enrollment has risen steadily over time. Today, slightly more than half of eligible beneficiaries choose it, with special needs plans (SNPs)—Part C plans tailored for those with specific chronic conditions—comprising a growing share of enrollment.
If you’re considering Medicare Part C (or just want to know if you should), read on. I’ll explain how Medicare Part C works, how it compares to Original Medicare, what its enrollment periods look like, and more.
Featured Financial Products
The information and analysis contained within this article appears for your consideration, but it does not constitute individualized financial advice. Always act at your own discretion.
How Does Medicare Part C Work?
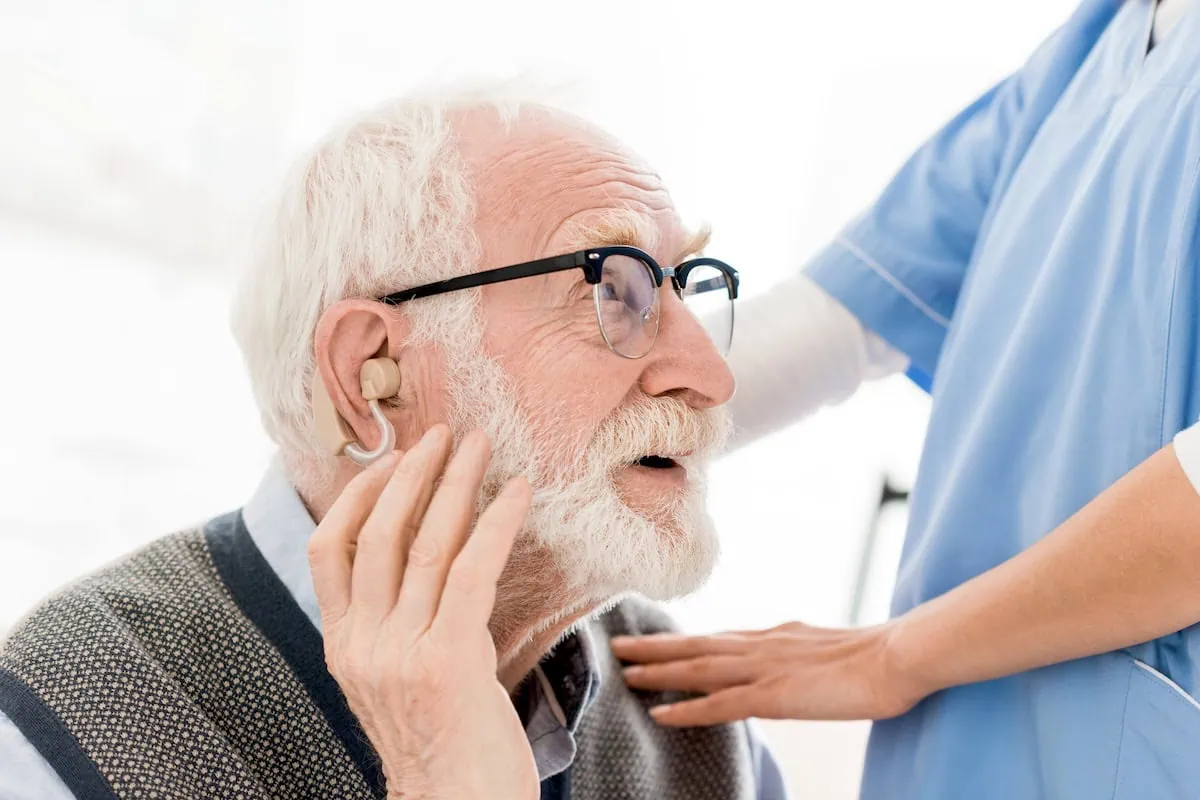
Medicare Part C plans are provided by private insurers. People can choose among a variety of plans with different benefits and pricing.
Medicare Advantage plans cover the services people get from both Medicare Part A (hospital insurance) and Medicare Part B (medical insurance). However, Part C also provides for other costs that Original Medicare doesn’t cover, such as prescription drugs, dental care, hearing care, and more.
Do you want to get serious about saving and planning for retirement? Sign up for Retire With Riley, Young and the Invested’s free retirement planning newsletter.
How Does Medicare Advantage Compare to Original Medicare?
We’re written in length about the differences between Original Medicare and Medicare Advantage, but here’s a brief recap of the most important points:
| Original Medicare (OM) | Medicare Advantage (MA) | |
|---|---|---|
| Coverage | Parts A and B. | Parts A and B. Can also include Part D (prescription), as well as other benefits, such as dental, hearing, and vision. |
| Drug Coverage | Must also enroll in Part D. | Is part of many MA plans. |
| Medigap | You can pair OM with Medigap. | You cannot use Medigap. |
| Provider Flexibility | Any provider that accepts Medicare. | Often requires you to stay in-network, may be geographically limited. |
| Specialist referrals | Typically not required. | Often required. |
| Out-of-pocket spending | No annual limit unless you have supplemental coverage like Medicaid or certain Medigap plans. | All plans have annual limits. |
| Premiums | You pay monthly premiums for Part A (if necessary) and Part B. Part D, if you enroll, is an additional premium. | You pay both the plan premium and the Part B premium. However, your plan premium might be free, and the plan might even pick up some of the Part B premium. |
One important similarity between the two? If you face financial difficulty and need ways to reduce your Medicare expenses, you might qualify for Medicare Savings Programs (MSPs), which are state-provided programs that help people pay for Part A and Part B premiums. MSPs can be used whether you have Original Medicare or Medicare Advantage.
Related: Medicare FAQs: Your Questions Answered
How Much Does Medicare Advantage Cost?
The projected 2026 average premium for Part C plans is $14 per month, per data from the Centers for Medicare and Medicaid Services (CMS).
Again, those with Medicare Advantage pay their chosen plan’s premium as well as Part B’s monthly premium, but some Part C plans have a $0 premium and may even help cover part or all of the Part B premium.
Part C deductibles vary widely depending on the chosen plan—you could expect anywhere from $0 to over $1,000. Similarly, coinsurance rates vary by plan.
Related: Healthcare Costs in Retirement [Amounts & Types to Expect]
When Should You Enroll in Medicare Part C?
Even though Part C provides the coverage you get from Parts A and B, you still need to be enrolled in A and B (as well as live within your chosen plan’s service area) to be eligible for Part C.
There are three types of enrollment periods for Original Medicare:
- Initial Enrollment Period (IEP): Your IEP lasts seven months. It starts three months before you turn 65 and ends three months after the month you turn 65. But if your birthday lands on the first of the month, then your IEP begins four months before you turn 65 and ends two months after the month you turn 65.
- The IEP applies not only to Original Medicare, but also Medicare Advantage and Part D.
- If you enroll in a Part C plan during this time, you’re permitted to drop it within 12 months and change to Original Medicare without penalty.
- General Enrollment Period (GEP): This three-month period, from Jan. 1 to March 31 each year, allows you to sign up for Parts A and/or B. (You might pay a monthly late enrollment penalty if you sign up during these dates.)
- If you have Medicare Part A, and you enroll in Part B for the first time during the GEP, that triggers a two-month Special Enrollment Period (SEP) in which you can enroll in Part C or Part D. If you don’t have Part A and you enroll in Part B, that triggers a two-month SEP in which you can enroll in Part D.
- Special Enrollment Period (SEP): In general, SEPs are one-time enrollment periods triggered by some sort of event. Depending on the event, you may have the opportunity to join Original Medicare, or a Medicare drug plan, or Medicare Advantage—some events apply to only one, some to two, and some to all three. Types of events that trigger a SEP for Medicare Part C include:
- Getting a chance to join coverage through an employer or union
- Having a plan whose contract with Medicare changes
- Losing current health care coverage
- Moving to a new location
Related: Don’t Overpay for Medicare: How to Avoid the Late Enrollment Penalty
Now that we’ve discussed the enrollment periods pertinent to Part A and Part B, there are two more to discuss that are relevant to Part C:
- Open Enrollment Period (OEP): The OEP runs from Oct. 15 to Dec. 7 every year. Within this period, people can enroll in, drop, or change Part C and/or Part D plans. Changes generally take effect on Jan. 1 of the following year.
- Medicare Advantage Open Enrollment Period (MA-OEP): The MA-OEP is from Jan. 1 to March 31, or within the first three months in which you get Medicare. People already enrolled in a Medicare Advantage Plan can use this time to make changes from their existing plans or switch to Original Medicare (and if you want, Part D as well).
Make sure you sign up for The Weekend Tea, Young and the Invested’s free weekly newsletter that over 10k monthly readers use to level up their money know-how.
More From Our Medicare 101 Series
- How Does Medicare Part A Work?
- How Does Medicare Part B Work?
- How Does Medicare Part D Work?
- How Does Medigap Work? Our Guide to Medicare Supplemental Insurance






![Here’s How You Can Lose Medicare [And How You Won’t] 7 how you can lose medicare](https://youngandtheinvested.com/wp-content/uploads/how-you-can-lose-medicare-600x403.webp)

